
Itch with Uncommon Diagnosis
Itch with Uncommon Diagnosis
What describes you and your itch?
Curious about itch Itch with Common Diagnosis Itch with Uncommon Diagnosis
Prurigo Nodularis
About Prurigo Nodularis
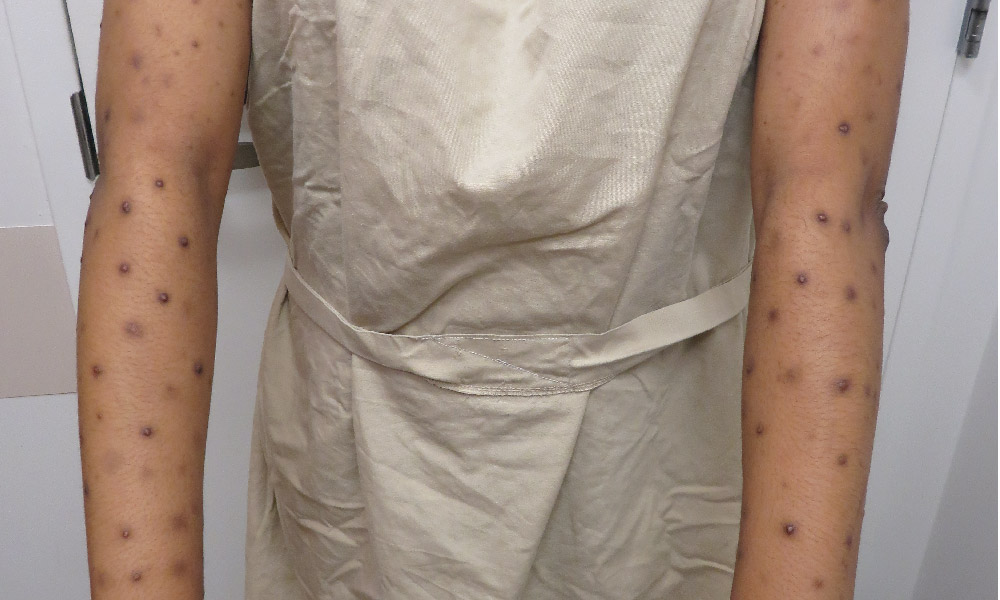 What Causes Prurigo Nodularis?
What Causes Prurigo Nodularis?
Though the exact cause of the condition is unknown, the nodules are the result of persistent, intense scratching or rubbing of the skin. The cause of prurigo nodularis is likely multifactorial and includes sensitivity to itch, inflammation, genetic predisposition, and environmental factors. A central component of this condition includes abnormalities in nerves and their signaling pathways. Individuals with prurigo nodularis may have increased sensitivity and heightened response of nerve fibers in the skin to various stimuli, leading to persistent itching. Imbalances in neurotransmitters and neuropeptides may also further transmission of these itch signals. Additionally, impaired skin barrier function can also make the skin more vulnerable to external irritants and allergens, further exacerbating the itching and scratching cycle. Immune dysregulation also plays a contributing role in prurigo nodularis, as research has identified increased levels of inflammatory mediators such as cytokines and chemokines in the skin lesions of these patients. Finally, an emerging concept is that nerves can directly promote inflammation through the release of neuropeptides; this is referred to as neuroinflammation.
How is Prurigo Nodularis Treated?
For patients with a limited number of nodular lesions, topical corticosteroids or topical calcineurin inhibitors can be used. These medications suppress the immune response in the skin. Other topical therapies that have been used with some success in patients with limited prurigo nodularis include topical capsaicin and anesthetics, which reduce the transmission of itch sensation in the nerve. However, oftentimes widespread or severe disease requires systemic therapy. Dupilumab, an immune-modulating biologic medication, is the first FDA-approved drug for prurigo nodularis and should be given as a first-line treatment for patients with severe disease. Other systemic therapies include immunosuppressants such as methotrexate or cyclosporine, thalidomide, and neuromodulators including gabapentin. Given the chronic and distressing nature of this condition, psychological support can also be beneficial in managing stress, anxiety, and depression associated with prurigo nodularis.
Common Myths about Prurigo Nodularis
“Scratching or picking at the nodules causes prurigo nodularis”
Scratching or picking at nodules is a symptom of prurigo nodularis rather than the cause. The condition arises from multiple factors including nerve abnormalities, immune system dysregulation, and inflammatory processes. The resulting itching and subsequent scratching can exacerbate the condition, leading to the formation of nodules.
“Prurigo nodularis is just a severe form of eczema”
Although prurigo nodularis shares some similarities with eczema, it is a distinct condition. Prurigo nodularis is characterized by the formation of nodules or bumps on the skin, often resulting from persistent scratching or rubbing. It is typically resistant to conventional eczema treatments and requires specialized management.
“Prurigo nodularis is only a skin problem”
Prurigo nodularis is a complex disorder involving interactions between the skin, nervous system, immune system, and potentially other physiological factors. The intense itching and chronic scratching associated with the condition can have a significant impact on an individual’s quality of life, leading to emotional distress, sleep disturbances, and even social isolation.
Uremic Pruritus
About Uremic Pruritus
 Uremic pruritus, also known as chronic kidney disease-associated pruritus, is a distressing symptom commonly experienced by individuals with advanced kidney disease.
Uremic pruritus, also known as chronic kidney disease-associated pruritus, is a distressing symptom commonly experienced by individuals with advanced kidney disease.
What Causes Uremic Pruritus?
Uremic pruritus is a complex condition that arises as a consequence of kidney dysfunction and the accumulation of various substances in the bloodstream. While the exact cause of uremic pruritus is not fully understood, multiple factors may contribute to its development. One factor includes alterations in the skin barrier, as kidney disease may cause water loss and reduced moisture retention in the skin. This dryness and disruption of the skin barrier can sensitize the skin, promoting itching. In addition to these changes, kidney disease can result in impaired filtration and accumulation of uremic toxins in the bloodstream, which can stimulate nerve endings and provoke itching. Chronic inflammation associated with kidney disease also plays a significant role in uremic pruritus. Individuals with this condition often exhibit elevated levels of pro-inflammatory molecules, which can further activate itch-specific nerves and contribute to itching.
How is Uremic Pruritus Treated?
Treating uremic pruritus requires a comprehensive approach that includes management of the underlying kidney disease. However, there are also specific interventions that may help alleviate itching and improve quality of life. For patients on dialysis, adjusting the dialysis regimen, such as increasing frequency or duration of sessions, may reduce itching by removing uremic toxins more efficiently. Topical treatments like adequate moisturization and emollients also help to restore skin hydration to alleviate itching. Topical corticosteroids can also help reduce inflammation and itching when applied to affected areas. Phototherapy can help alleviate the itch, presumably through its anti-inflammatory effects as well. For severe or recalcitrant itching, gabapentin, a neuromodulator, should be considered. Difelikefalin is an opioid receptor modulator and the first FDA-approved drug for uremic pruritus in kidney disease patients undergoing dialysis. This should be immediately considered in anyone with dialysis-associated uremic pruritus.
Common Myths about Uremic Pruritus
“Uremic pruritus is a common symptom in all individuals with kidney disease.”
Although uremic pruritus occurs in individuals with advanced kidney disease, it is not experienced by every person with kidney disease. The prevalence of uremic pruritus varies among individuals and factors such as the severity of kidney dysfunction.
“Uremic pruritus will resolve once kidney function improves”
Uremic pruritus may persist even after kidney function improves through interventions such as dialysis or transplant. Thus, effective management strategies focus on also providing relief from itching and improving overall well-being.
“Uremic pruritus is not serious because patients have more serious things to worry about”
Studies show that even patients with cancer care tremendously about quality of life, and not just extension of life. Pruritus is a major concern among patients that goes routinely overlooked by providers.
Chronic Pruritus of Unknown Origin
About Chronic Pruritus of Unknown Origin
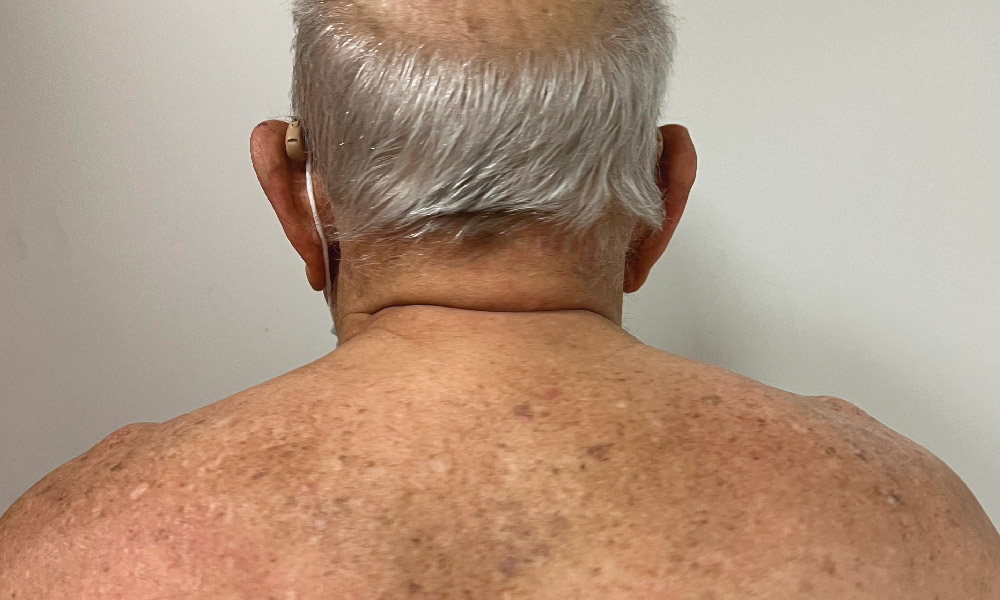 Chronic pruritus is defined as itch lasting greater than 6 weeks. When the underlying cause of itch cannot be identified, it is known as chronic pruritus of unknown origin (CPUO). This condition most commonly occurs in the elderly.
Chronic pruritus is defined as itch lasting greater than 6 weeks. When the underlying cause of itch cannot be identified, it is known as chronic pruritus of unknown origin (CPUO). This condition most commonly occurs in the elderly.
What Causes CPUO?
CPUO can be diagnostically challenging as all known chronic itch disorders and underlying diseases should be excluded prior to diagnosis. While the exact cause of CPUO has not been elucidated, several mechanisms are thought to contribute to this condition. One prevailing hypothesis is that CPUO arises from increased sensitivity of itch-specific nerves and changes in the neural signaling pathways may cause increased transmission of itch sensations. Inflammation is also thought to play a role in CPUO, even when no rash is evident. Low-grade inflammation in the skin or body, often associated with senescence of the healthy immune system, may result in increased levels of particular immune cells and inflammatory mediators which can trigger itch signals. Furthermore, disruptions of the skin barrier function whether due to age, genetic factors, environment, or underlying skin conditions, can cause skin dryness and increased susceptibility to irritants and allergens.
How is CPUO Treated?
While there are currently no FDA-approved medications for CPUO, general anti-itching therapies are helpful for the management of associated symptoms. Several strategies can help manage and alleviate itching. If itching is mild or limited to small areas on the skin, topical menthol, capsaicin, or anesthetics may help to reduce transmission of itch sensation through the nerves. For severe or widespread itching, systemic therapies including neuromodulatory agents like gabapentin, opioid receptor modulators such as butorphanol and naltrexone, and newer biologic agents including dupilumab or tralokinumab or JAK inhibitors like abrocitinib and upadacitinib should be considered by your doctor.
Common Myths about CPUO
“CPUO is simply a manifestation of dry skin”
While dry skin can contribute to itchiness, CPUO encompasses a range of complex factors beyond dryness alone. It is a multifaceted condition involving neural hypersensitivity, inflammation, skin barrier dysfunction, and other underlying mechanisms.
“CPUO is just caused by stress”
Although psychological factors can influence itch perception and exacerbate symptoms, CPUO is not purely stress-related. It has biological and physiological underpinnings, involving neural, immune, and inflammatory pathways. Psychological factors may contribute to the intensity and persistence of itch, but they are not the sole cause of the condition.
“CPUO is a rare condition”
CPUO is more common than often perceived. It can affect individuals of any age, although it is most prevalent in the elderly. The true prevalence is difficult to estimate due to variations in diagnostic criteria and underreporting. However, many individuals experience chronic itch without an identifiable cause, highlighting the need for greater awareness and understanding of this condition.
Notalgia Paresthetica
About Notalgia Paresthetica
 Notalgia paresthetica is characterized by itching or tingling sensations between the shoulder blade and spine. The condition usually affects only one side of the back but can also affect both sides.
Notalgia paresthetica is characterized by itching or tingling sensations between the shoulder blade and spine. The condition usually affects only one side of the back but can also affect both sides.
What Causes Notalgia Paresthetica?
Notalgia paresthetica is caused by compression, irritation, or damage of the nerves from the spine. Compression of nerves in the upper back region can result from various factors such as degenerative changes in the spine, spinal injury, or anatomical variations in the surrounding structures. Poor spinal alignment or posture may also contribute to nerve compression or irritation in the upper back region. The symptoms of notalgia paresthetica often follow a specific distribution in the skin that corresponds to a particular area of skin supplied by corresponding spinal nerves.
How is Notalgia Paresthetica Treated?
The management of notalgia paresthetica centers on alleviating symptoms. Physical therapy may help improve spinal alignment and address muscular imbalances. Other treatments such as transcutaneous electrical nerve stimulation (TENS) are thought to help numb the nerves for temporary itch relief. Topical therapies, such as capsaicin cream or patches and menthol-based ointments, may also provide temporary relief from itching. In some cases, oral neuromodulators such as gabapentin may be prescribed to help manage symptoms. Interventional procedures including nerve blocks or corticosteroid injections may be considered for severe cases. Newer therapies are also currently under development in upcoming clinical trials for notalgia paresthetica.
Common Myths about Notalgia Paresthetica
“Notalgia paresthetica is a rare condition”
Notalgia paresthetica is often underdiagnosed, leading to the misconception that it is a rare condition. However, it is believed to be more common than currently recognized.
“Notalgia paresthetica is not a serious condition”
While notalgia paresthetica is not life-threatening, the condition can significantly impact quality of life. Symptoms may range from mild to intense, and the chronic itching and discomfort is often distressing for individuals with notalgia paresthetica.
“Notalgia paresthetica only affects the elderly”
While notalgia paresthetica is more common in middle-aged and older individuals, the condition may affect individuals of any age, including younger adults, especially those with a history of neck or spine injuries.
What is Itch & Scratch?

Itch is a sensation that many people experience yet don’t understand. The philosopher Aristotle (384-322 BC) recorded one of the first known descriptions of itch, characterizing how animals scratch themselves in a manner similar to modern humans.




