
Itch with Common Diagnosis
Itch with Common Diagnosis
What describes you and your itch?
Curious about itch Itch with Common Diagnosis Itch with Uncommon Diagnosis
Eczema
About Eczema
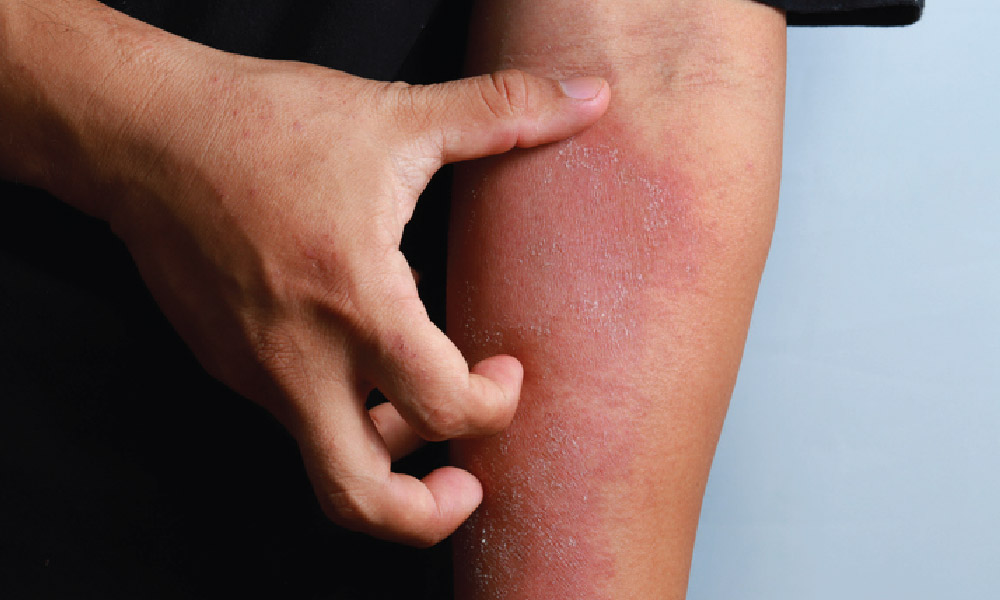 If you suffer from itchy, flaky, red skin that won’t seem to go away no matter how much lotion you use, you may be among the millions of people globally who are living with eczema, a chronic skin condition also known dermatologically as atopic dermatitis. Eczema may affect any part of the body, but tends to occur on the face, hands, and creases of the elbows and knees. People with eczema often experience dryer skin that may be sensitive to certain triggers such as heat or stress.
If you suffer from itchy, flaky, red skin that won’t seem to go away no matter how much lotion you use, you may be among the millions of people globally who are living with eczema, a chronic skin condition also known dermatologically as atopic dermatitis. Eczema may affect any part of the body, but tends to occur on the face, hands, and creases of the elbows and knees. People with eczema often experience dryer skin that may be sensitive to certain triggers such as heat or stress.
What Causes Eczema?
The cause of eczema is complex and multifactorial, involving elements of genetic predisposition, alterations in immune responses, and environmental factors. Genetics play an important role in determining one’s risk for developing this condition. Approximately 50 percent of individuals with eczema have mutations in the FLG gene that causes cells to produce less filaggrin. This loss compromises the upper layers of the skin, resulting in uncomfortable, dry skin that is prone to infection and allergic reactions. Overactive or dysregulated immune function can also contribute to eczema and promote skin hypersensitivity. Additionally, chemicals such as harsh detergents, fragrances, and certain skin care products can alter the skin’s pH and trigger inflammation. Environmental pollutants can also promote an immune response to further aggravate eczema. Finally, exposure to extreme temperatures or overly dry air can exacerbate existing causes or even increase the risk of developing eczema.
How Is Eczema Treated?
Treatment of eczema involves avoiding potential triggers and using prescription creams or ointments alongside other lifestyle changes such as moisturizing well and avoiding long hot showers or baths. Light therapy may also be effective for people who are not able to manage their eczema with topical treatments or experience rapid flare-ups after treatment. If topical treatments are not adequate in treating your eczema, your doctor may also prescribe oral medications such as steroids and immunosuppressants. However, newer treatments are available, rendering the latter to be less relevant. Recently, injectable biologics such as dupilumab and tralokinumab received FDA approval for moderate to severe eczema, providing greater therapeutic options.
Common Myths About Eczema
“Eczema is contagious”
This is not true since eczema is not caused by an infection nor spread through contact between people like colds or viruses do. While secondary infections can occur if open sores become infected due to frequent scratching without proper treatment, eczema itself is not a contagious condition.
“Only children get eczema”
While eczema is more common in children, adults can also experience the condition, especially if they previously experienced eczema in childhood.
“Eczema can be treated with any lotion”
While proper moisturization with the right products can help protect a fragile or damaged skin barrier in eczema, not all moisturizing creams are effective and can even cause irritation. Products containing ingredients such as fragrances, essential oils, retinol, and ethanol can actually aggravate eczema. As a result, it is often helpful to consult the ingredients list prior to trying a new skincare product.
Hives
About Hives
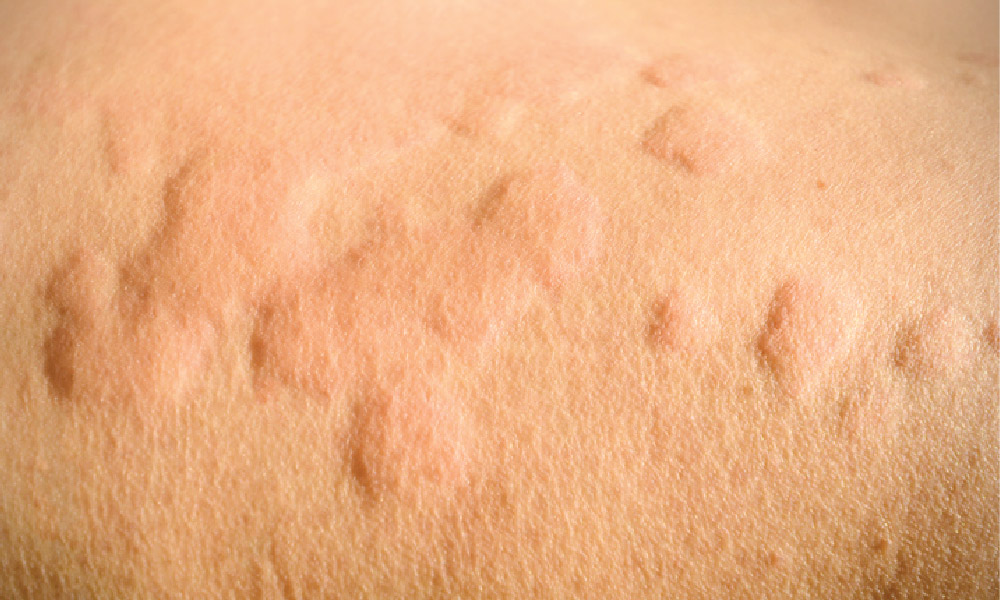 Hives, also known as urticaria, are characterized by raised red and itchy welts on the skin that can be uncomfortable and even painful for those who suffer from it. Hives affect up to 20 percent of people and can be triggered by foods, medications, insect bites, physical stimuli, temperature, and allergens, among others. While many causes of hives are short-term and mild in nature, some individuals may experience chronic or severe forms of the condition.
Hives, also known as urticaria, are characterized by raised red and itchy welts on the skin that can be uncomfortable and even painful for those who suffer from it. Hives affect up to 20 percent of people and can be triggered by foods, medications, insect bites, physical stimuli, temperature, and allergens, among others. While many causes of hives are short-term and mild in nature, some individuals may experience chronic or severe forms of the condition.
What Causes Hives?
Hives are formed when the body releases histamine (and other factors) stored within your immune cells. When your immune system responds to potential threats such as food proteins or foreign chemicals entering the body, histamine is released to promote swelling, itching, and inflammation. However, sometimes the immune system releases histamine when there is no real threat, such as in allergic reactions. While hives typically resolve within a few hours to days with no lasting consequences, chronic hives, defined as lasting almost daily for more than 6 weeks, can be frustrating and significantly affect your quality of life. In chronic spontaneous urticaria (CSU), hives and itch may come and go unexpectedly with no known cause. Many of these patients have an underlying process whereby their own antibodies have developed a reactivity that triggers mast cells, a type of immune cell, to release histamine and other factors. Another example is chronic inducible urticaria (CIndU) whereby patients experience hives and itching in response to heat, cold, pressure, vibration, and a variety of other neurologic triggers. An emerging family of disorders referred to as mast cell activation syndrome (MCAS), is caused by overproduction of certain inflammatory molecules within mast cells, that make them prone to releasing higher levels of histamine and other proinflammatory mediators.
How are Hives Treated?
Hives can range from mild to severe and usually come and go suddenly without lasting long-term effects. Treatment for hives depends on its severity but typically includes antihistamines taken orally. If hives do not respond well enough to these medications, your doctor may consider starting biologic injections such as omalizumab or immunosuppressants to target overactive inflammatory pathways. Alongside therapeutic options, avoiding potential triggers may help in reducing or preventing hives.
Common Myths
“All hives are due to allergies”
It has long been thought that hives occur due to an allergic reaction caused by antibodies produced by the immune system responding to foreign substances like food proteins or chemicals entering the body. However recent research suggests there may be more than one mechanism at work when it comes to these outbreaks of skin irritation. For instance, your body can develop antibodies against your own cells. Another cause for hives is mast cell activation syndrome (MCAS), which occurs when activated mast cells release histamine into the bloodstream too quickly and in large amounts, resulting in inflammation throughout the body and triggering symptoms such as itching and swelling. This excessive release of histamine causes blood vessels near the surface of your skin to dilate leading to increased blood flow which further contributes towards reddening and inflammation seen on affected areas during bouts with hives. MCAS is believed to arise from genetic mutations inherited from either parent causing overproduction of certain inflammatory molecules within mast cells making them prone to frequent degranulation events releasing higher levels of pro-inflammatory mediators like cytokines, chemokines, and leukotrienes, leading towards the development of hive episodes. Another potential factor associated with this condition could be dysregulation between different signaling pathways involved in controlling the activity levels of specialized white blood cells.
“Hives are a sign of a severe medical condition”
While hives can be distressing and uncomfortable, they are often harmless and temporary. Acute hives usually resolve within a few hours to a few days without any lasting effects. However, chronic hives that persist for more than six weeks can sometimes be indicative of an underlying health issue and may require further evaluation and treatment with your doctor.
“Hives can only appear on the skin”
Although hives primarily manifest as raised welts on the skin, they can also affect deeper tissues such as the lips, throat, and even internal organs. When hives involve the throat or tongue, they can cause swelling and potentially lead to breathing difficulties. This condition, known as angioedema, requires immediate medical attention.
Lichen Planus
About Lichen Planus
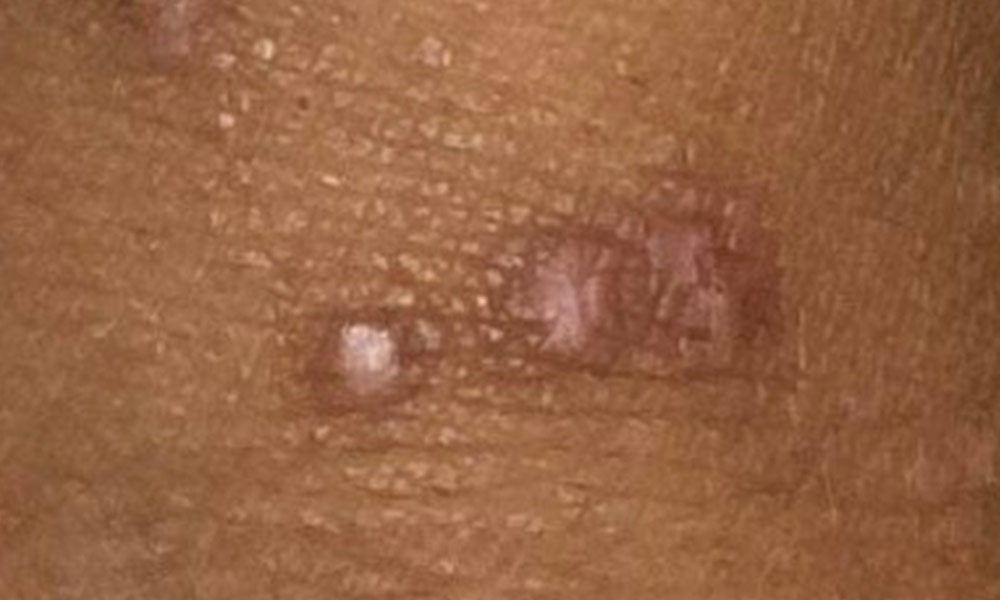 Lichen planus is a relatively common chronic inflammatory skin condition that affects millions of people worldwide. Although this condition may occur in all age groups, women over the age of 50 years are most commonly affected.
Lichen planus is a relatively common chronic inflammatory skin condition that affects millions of people worldwide. Although this condition may occur in all age groups, women over the age of 50 years are most commonly affected.
What Causes Lichen Planus?
Lichen planus presents as a rash, affecting various areas of the body, including the skin, mucous membranes, hair, and nails. The condition is characterized by itchy, reddish-purple bumps or papules with distinctive white lines or patterns, resembling lichen growing on rocks. Lichen planus is an immune-mediated disorder. It is believed that certain factors trigger an abnormal immune response, leading to inflammation and damage to the skin and mucous membranes. Various immune cells, including T lymphocytes, have been implicated in initiating and perpetuating this inflammatory process. In addition, genetic predisposition may play a contributing role. Certain genes associated with human leukocyte antigen (HLA), which are involved in immune system regulation, are associated with an increased risk of developing the condition. Aside from immune dysregulation and genetic components, environmental factors may act as triggers for lichen planus in susceptible individuals. These triggers can include viral infections (such as hepatitis C), certain medications (including nonsteroidal anti-inflammatory drugs), and stress. However, it is important to note that not everyone exposed to these triggers will develop lichen planus, highlighting the complex interplay between genetics, immune system, and environmental factors.
How is Lichen Planus Treated?
The treatment of lichen planus aims to alleviate symptoms, reduce inflammation, and promote healing. Topical corticosteroids are commonly used as a first-line treatment to reduce inflammation and itching. Topical calcineurin inhibitors can also be prescribed as an alternative to corticosteroids for sensitive areas or long-term use. These medications work by suppressing the immune reaction in your skin. In more severe cases or when topical treatments are not sufficient, oral corticosteroids may be prescribed by your doctor. While these medications can help control inflammation throughout the body, they are typically only used for short periods due to their potential side effects. Other systemic therapeutic option includes oral retinoids which can be used to reduce inflammation and immunosuppressive agents such as methotrexate. Phototherapy may also be recommended by your doctor as a treatment or in addition to another therapy.
Common Myths about Lichen Planus
“Lichen Planus is a contagious condition.”
Lichen planus is not a contagious condition. It cannot be transmitted through direct contact, sharing personal items, or being in close proximity to someone with lichen planus. It is an autoimmune disorder that arises from an abnormal immune response and is not caused by bacteria, viruses, or other infectious agents.
“Lichen planus is caused by poor hygiene.”
Lichen planus is not caused by poor hygiene practices. It is an immune-mediated condition that occurs due to an abnormal immune response, not due to a lack of cleanliness. Maintaining good hygiene practices is important for overall skin health, but it does not prevent or cause lichen planus.
“Lichen planus only affects older individuals.”
Although lichen planus is more commonly seen in middle-aged and older adults, it can affect individuals of any age, including children and adolescents. The prevalence and severity of lichen planus may vary among different age groups, but it is not exclusively limited to older individuals.
Allergic Contact Dermatitis
About Allergic Contact Dermatitis
 This type of skin irritation occurs when the body has an allergic reaction to a substance that comes into contact with the skin. It typically presents as red, swollen, and itchy skin eruptions.
This type of skin irritation occurs when the body has an allergic reaction to a substance that comes into contact with the skin. It typically presents as red, swollen, and itchy skin eruptions.
What Causes Allergic Contact Dermatitis?
Allergic contact dermatitis (ACD) can be caused by contact with cosmetics, jewelry, clothing materials, or plants such as poison ivy. While anyone can develop an allergic reaction to any allergen on the skin surface, some people are more prone to developing ACD due to genetics or environmental factors. Understanding the science behind ACD requires knowledge of how the immune system works in response to foreign substances coming into contact with our body’s surfaces. When these foreign substances come into contact with the skin surface, they encounter immune cells located at the skin surface. These immune cells can then cause your white blood cells to become sensitized and elicit a localized inflammatory response, resulting in itching and swelling.
How is Allergic Contact Dermatitis Treated?
While ACD may not require medical treatment, individuals who suffer from recurrent bouts of ACD should first identify what specific allergens may be underlying their symptoms in order to avoid further exposure. Anti-itch creams or ointments such as hydrocortisone or calamine lotion may help reduce itching.
Common Myths about Allergic Contact Dermatitis
“ACD is the same as irritant contact dermatitis”
While both conditions involve skin inflammation, they are two distinct conditions. ACD specifically refers to an allergic reaction triggered by contact with an allergen, whereas irritant contact dermatitis is caused by inflammation from repeated exposure to an irritant. The mechanisms and treatment approaches for ACD and irritant contact dermatitis also differ.
“ACD is always caused by exposure to a new substance”
A common misconception is that ACD occurs only when exposed to a new substance. In reality, ACD typically develops after repeated exposure to a substance that a person has previously tolerated. Sensitization to an allergen can occur over time, and individuals may develop an allergic reaction to a substance they have previously encountered without any issues.
“ACD only affects the area of direct contact”
While ACD typically manifests as a localized rash at the site of contact, it is possible for the reaction to spread beyond the initial contact area. The allergen may sometimes be transferred to other parts of the body through touch, causing a more widespread rash or allergic reaction.
What is Itch & Scratch?

Itch is a sensation that many people experience yet don’t understand. The philosopher Aristotle (384-322 BC) recorded one of the first known descriptions of itch, characterizing how animals scratch themselves in a manner similar to modern humans.




